The United States has recorded its highest number of measles cases in more than three decades, with 1,288 infections confirmed so far in 2025, according to the latest data from the U.S. Centers for Disease Control and Prevention (CDC). The figure marks the worst outbreak since 1992—eight years before the disease was declared eliminated in the U.S.—and has triggered renewed concern among public health experts.
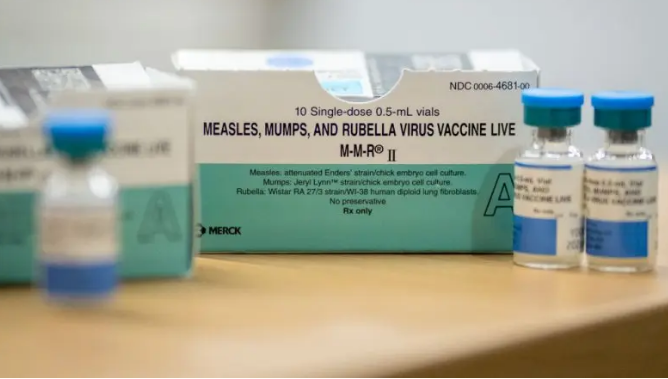
Measles, one of the most contagious viruses known, is preventable through the measles, mumps, and rubella (MMR) vaccine. But a steady decline in vaccination rates has left communities increasingly vulnerable. The CDC reports that 92% of this year’s cases occurred in individuals who were either unvaccinated or whose vaccination status is unknown.
Experts warn that this surge could be a harbinger of wider trouble.
“This was expected—but still alarming,” said epidemiologist Katelyn Jetelina. “We’re at a turning point. Measles is the first to reappear when vaccination coverage slips, but it won’t be the last.”
Indeed, the drop in immunization rates is raising red flags across the public health sector. The CDC reported that MMR vaccination coverage among kindergartners fell to 92.7% during the 2023–2024 school year—below the 95% threshold required to maintain herd immunity.
The decline is attributed to multiple factors, including rising vaccine hesitancy during the COVID-19 pandemic and growing influence of vaccine skeptics. The issue has been further inflamed by recent decisions under Health and Human Services Secretary Robert F. Kennedy Jr., a known critic of vaccines. Kennedy recently disbanded the CDC’s vaccine advisory committee and replaced it with individuals who have expressed skepticism about immunizations. The new panel has already voted to halt recommendations for certain flu vaccines and is reviewing the childhood vaccination schedule.
The broader implications of such moves are concerning, say experts. Michael Osterholm, director of the Center for Infectious Disease Research and Policy (CIDRAP), warned that diseases like mumps, rubella, and whooping cough could be next.
“We’re at risk of undoing decades of progress,” he said. “If vaccination rates keep falling, more children will fall seriously ill—and some will die.”
Already this year, three measles-related deaths have been confirmed, including two young girls in Texas. CDC data show that 13% of measles patients were hospitalized, with the rate rising to 21% among children under five.
Dr. Paul Offit of the Children’s Hospital of Philadelphia stressed the deadly reality of the disease: “Those two girls were perfectly healthy. Measles can kill anyone.”
Beyond the immediate health crisis, experts view the resurgence as a symptom of deeper issues. “This isn’t just about measles,” Jetelina said. “It’s about a breakdown of trust, rising individualism over collective health, and systems buckling under disinvestment.”
With measles emerging as a symbol of eroding public health protections, officials and experts alike are urging a renewed commitment to immunization—and to restoring confidence in science.