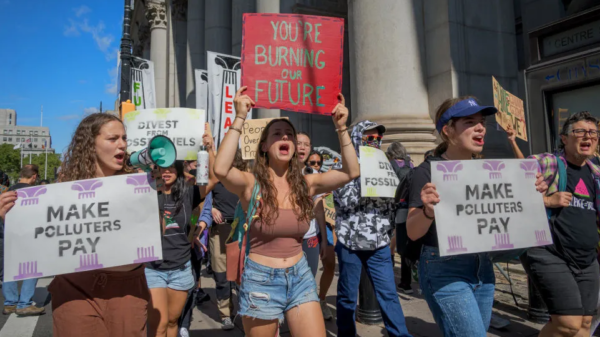New research has found that U.S. veterans with both insomnia and sleep apnea face significantly higher risks of high blood pressure and heart disease, highlighting the long-term health consequences of disrupted sleep.
The study, published in the Journal of the American Heart Association, followed nearly one million post-9/11 veterans over two decades, examining the connection between sleep problems and cardiovascular health. Those with both disorders were found to have more than twice the risk of developing high blood pressure and over four times the risk of heart disease compared with veterans without sleep disorders. While the research does not explain the exact mechanisms, experts say the findings reinforce the importance of sleep for long-term heart health.
The analysis drew on medical records from the Department of Veteran Affairs, a large and detailed database that provided insight into the health of a population known to have higher rates of sleep disorders. “Veterans experience elevated sleep issues due to deployment-related stress, irregular schedules, PTSD, depression, anxiety, physical injuries, and chronic pain,” said Allison Gaffey, a clinical health psychologist at Yale School of Medicine and one of the study’s authors. She added that veterans also have higher rates of heart disease, raising questions about whether addressing sleep problems could improve cardiovascular outcomes.
The study’s results surprised researchers because the participants were relatively young, with over 40% under the age of 40 when they first enrolled in VA services. The increase in heart risk appeared across both men and women. “We often think of cardiovascular disease as a concern for later in life,” Gaffey said. “But the foundation for heart health begins much earlier, and chronic sleep disruption can influence cardiovascular risk far sooner than typically recognized.”
Experts note that treating sleep disorders is complex. Obstructive sleep apnea is typically managed with a continuous positive airway pressure (CPAP) machine, while cognitive behavioral therapy (CBT-I) is the standard treatment for insomnia. Peter Catcheside, a sleep and respiratory physiologist at Flinders University in Australia, said studies suggest addressing insomnia with CBT-I before starting CPAP can be more effective than the reverse. He added that understanding the root cause of sleep problems is critical, as apnea may sometimes be the underlying factor causing insomnia-like symptoms.
Gaffey emphasized the broader significance of the findings. “Sleep isn’t just about feeling rested,” she said. “It’s an active, restorative process, and chronic disruption has measurable consequences for cardiovascular health.” She urged anyone experiencing persistent difficulty falling or staying asleep, or daytime fatigue, to seek professional help, noting that early intervention could improve long-term health outcomes for both veterans and civilians.